Women and Cardiovascular Risk

Even during the pandemic, women need to watch their heart health
Always consult your health care provider with questions or concerns you may have regarding your health.
While it’s important to focus on staying safe during the pandemic, don’t ignore your biggest risk: heart disease. It’s the leading cause of death for women in the United States — responsible for 1 in 5 deaths.1 Nearly 46,000 women died from heart attacks in 2017.2
Surprised? You aren’t alone: In 2019, only 44% of women were aware that heart disease is their leading cause of death, the American Heart Association (AHA) reports.3 That’s down from 65% in 2009.3


But with COVID-19 and everything we’re doing to look out for family members and friends, it’s especially easy to lose track of heart health and ignore the warning signs for heart disease and heart attacks. Especially take note of the known signs and symptoms of heart attacks4,5:
- Chest discomfort. Most heart attacks involve discomfort in the center or left side of the chest that lasts more than a few minutes — or it may go away and then return. It can feel like uncomfortable pressure, squeezing, fullness or pain.
- Discomfort in other areas of the upper body. Symptoms can include pain or discomfort in one or both arms, the back, neck, jaw or stomach.
- Shortness of breath. This can occur with or without chest discomfort.
- Other signs. Other possible signs include breaking out in a cold sweat, nausea or lightheadedness or sudden dizziness.
- 1/3
- 2/3
- 3/3



“As with men, women’s most common heart attack symptom is chest pain or discomfort,” says Dr. Rosa Coppolecchia, Director of U.S. Medical Affairs Cardiology, Consumer Health at Bayer. “But women are somewhat more likely than men to experience some other common symptoms, particularly shortness of breath; pressure or pain in the lower chest and upper abdomen; dizziness, lightheadedness or fainting; upper back pressure; nausea or vomiting; extreme fatigue and back or jaw pain.”
Barriers to Heart Health for Women
In fact, despite the stereotype that heart disease is a “man’s issue,” 6.2% of women suffered from heart disease between 2013 and 2016 versus 7.4% of men, the AHA says in its 2020 update.2
Women face several barriers to heart health compared with men.
First, risk factors for heart disease increase when they reach menopause, with an overall increase in heart attacks about 10 years after menopause, the AHA says.6 Researchers suspect that the lower estrogen levels may contribute to the higher risk factors,6 which are1:
- High blood pressure
- Unhealthy cholesterol levels
- Smoking
- Diabetes
- Obesity
- Having an unhealthy diet
- Physical inactivity
- Drinking too much alcohol

Second, women might attribute some of the symptoms to other causes. For example, “with extreme fatigue, it’s difficult to differentiate between having a potential heart attack and being tired from having a long day or week,” Dr. Coppolecchia says.
Even the medical community has more difficulty diagnosing heart attacks in women: Compared with men, women are 50% more likely to be misdiagnosed after having a heart attack, according to a 2016 study from the University of Leeds in the U.K.7
Third, we don’t know enough about the differences between men and women regarding heart disease. “We have very limited studies on women and heart disease,” Dr. Coppolecchia says.
Women account for less than a third of all subjects in heart disease studies, according to a 2014 George Washington University report.8 And less than a third of cardiovascular disease clinical trials that include women report outcomes by sex.8
The medical community is working to better understand how heart disease affects women, Dr. Coppolecchia says, such as including more of them in clinical trials. For now, as the following two women can attest — both advocates for heart health through WomenHeart (a Bayer partner), a national patient advocacy organization for women with heart disease — the most important steps are for women to be mindful of their heart health and to pay close attention to the warning signs.
Two Stories of Survival and Hope
Sue Chlebek, La Porte, Indiana
By all accounts, Sue Chlebek should not be here today. The 50-year-old was living a healthy, active life and thought she was too young to worry about her heart. But on a sunny day 10 years ago, Sue drove herself to the ER after experiencing shortness of breath, followed by periodic quick, sharp chest pains.
Battling the voice that told her she was overreacting, Sue finally allowed herself to panic as another sharp pain arose. She ran the last red light and parked at the ER entrance.
- 1/5
- 2/5
- 3/5
- 4/5
- 5/5





Sue told the triage nurse she thought she was having a heart attack. Wary, the nurse replied, “Why do you think you’re having a heart attack?” Sue never answered. “I had sudden cardiac arrest and I was a code blue,” she recalls. “I woke up some time later on a different floor of the hospital. My first memory is thinking, ‘Am I dying?’ I didn’t know I’d already done that.”
What Sue did not realize is that her heart’s LAD (left anterior descending) artery was nearly completely blocked and required a stent. “So few people survive a heart attack in that artery,” says Sue, whose road to recovery — like many people’s after a heart attack — was long and challenging. Today, she sees her experience as a blessing. “I really believe, very strongly, that what I’m supposed to do is help other people live healthy lives, and especially women,” she says.
Women are often caregivers of children, spouses and parents. So many times, women put their health last. “We need to turn that around so that we can be there to take care of the people we love,” she says. “I can’t imagine where my little 5-year-old Sophie would have been without her mom.”
“The scary thing is, my symptoms were not that bad,” Sue adds. “Women need to know that. Some women have no chest pain at all.” Some think they have the flu; some have arm pain, nausea or shortness of breath. “You need to make sure you know the signs and symptoms of a heart attack.”
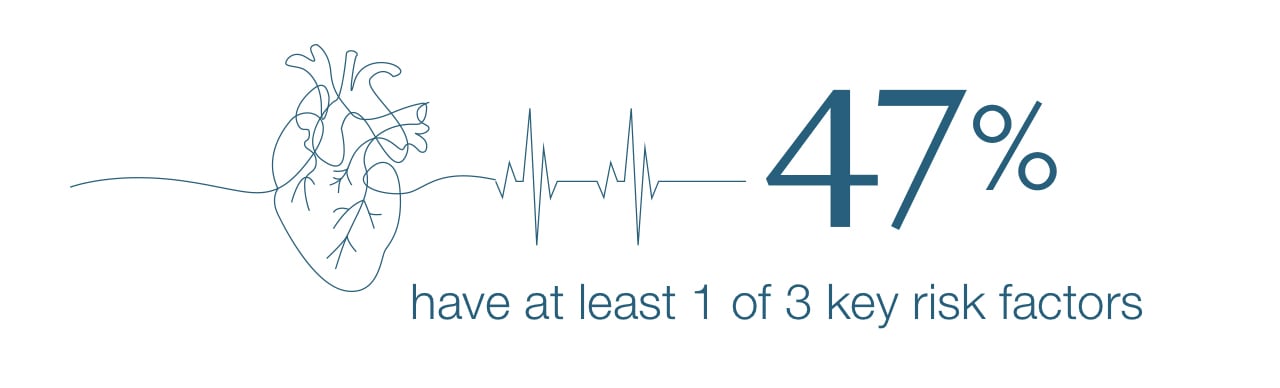
Women also need to know their family health history, if possible, and risk factors. “Stay on top of your health. Make sure you’re exercising and eating healthy. Know your numbers … your cholesterol and your blood pressure,” she says. About half of all Americans (47%) have at least one of three key risk factors for heart disease: high blood pressure, high cholesterol and smoking.1
“Be informed,” Sue adds. “Know your body. Know the symptoms. If it seems like something may not be right, trust yourself and go in.
“Don’t delay, especially now in COVID, because [heart disease] is still your No. 1 risk. This remains our No. 1 killer of all Americans and of women. Be aware and believe your body when it’s telling you something. Don’t take a chance. You can be perfectly fine one second and the next second, you can be gone. I am proof of that.”
Nichele Hoskins, Savannah, Georgia
Nichele Hoskins was 36 and teaching fitness classes when she first experienced heart symptoms. That same year, she was in a two-day 30-mile walk for breast cancer when she had her first heart event.
While Nichele had classic heart attack symptoms, doctors missed her diagnosis. “I had numbness, slight nausea and an unusual sense of anxiety,” she recalls. A physician told her, “You probably don’t have heart disease. It’s probably gas.” Fortunately, he scheduled a stress test. She was immediately admitted for an angioplasty, which revealed 80%–90% blockage in one artery. Since then, she’s experienced several more blockages.
- 1/5
- 2/5
- 3/5
- 4/5
- 5/5





Today, the lifetime fitness fan now sports seven heart stents. Fittingly, Nichele, now 53, is assistant director of Healthy Savannah and a strong advocate for women and heart disease. And she’s learned a lot about coping with her heart health.
Nichele had to get over the belief that heart disease was her fault. “We try to bear too much blame when genetics and other things have had an impact,” she explains. “The reality is, people who have heart attacks don’t necessarily look like the people you might expect.”
In addition, women’s symptoms can be very different from men’s, including indigestion, stomach flu–like symptoms and neck pain, she says. “I’ve known people who had lower back pain accompanied by awareness that something was different. If you’re familiar with some of the symptoms, err on the side of caution and get it checked.”
Don’t let your physician dismiss you, either, she says. “I’ve had to stand almost flat-footed in a doctor’s face and say, ‘This is what I’m feeling.’ Dismissive treatment is not acceptable. All those things make it necessary for us to be really vigilant … and have a sense of humor about it.”
That vigilance doesn’t end after a heart attack. As Nichele experienced, about one in five people who have had a heart attack are readmitted to the hospital for a second one within five years, the AHA says.9
Now is a critical time to stay on top of your health, she stresses. “Don’t neglect your medical care just because you’re trying to avoid COVID. My doctor’s office is being very careful about things. I wouldn’t ignore any symptoms.”

Don’t Let COVID-19 Keep You from the Doctor’s Office
Nichele’s words about getting proper medical care during the pandemic are what’s driving a partnership that includes Bayer and other companies, the CDC Foundation and the Million Hearts® initiative. The effort produced two public service announcements that reminded people to pay attention to their heart health, especially during COVID-19.
The partnership noted that people with cardiovascular disease are at heightened risk of complications from COVID-19.10 Meanwhile, people might delay seeking medical care if they had symptoms of serious heart problems because they feared contracting the virus.10 In fact, the CDC says in the 10 weeks after declaration of the COVID-19 national emergency, visits to emergency departments for heart attacks fell by 23% from normal levels.11

Control What You Can: Your Lifestyle
Besides making new treatments for heart failure a research priority, Bayer has introduced digital solutions to help patients with their drug-based treatments.12 Patients with atrial fibrillation, for example, can receive a daily text message reminding them to take their medication.12 Another effort focuses on sending data from patients directly to their physicians.12
Dr. Coppolecchia also admonishes people who are on medications to control high cholesterol, high blood pressure, diabetes or other conditions considered risk factors for heart disease to continue closely monitoring their heart health. Although the medications are helping control the risk factors, “you’re still high risk,” she says.
As the stories of Sue and Nichele illustrate, nobody can control all aspects of their health or know when heart emergencies will occur. But you can live a heart-healthy lifestyle through proper diet and exercise and heed the warning signs of most serious heart issues. Call 911 immediately if you experience any of the signs or symptoms of a suspected heart attack.
References
1 https://www.cdc.gov/heartdisease/women.htm
2 https://www.heart.org/-/media/files/about-us/statistics/women-ucm_505482.pdf?la=en
3 https://www.ahajournals.org/doi/10.1161/CIR.0000000000000907
4 https://www.cdc.gov/heartdisease/heart_attack.htm
5 https://www.goredforwomen.org/en/about-heart-disease-in-women/signs-and-symptoms-in-women/symptoms-of-a-heart-attack
6 https://www.heart.org/en/health-topics/consumer-healthcare/what-is-cardiovascular-disease/menopause-and-heart-disease
7 https://www.leeds.ac.uk/news/article/3905/heart_attacks_in_women_more_likely_to_be_missed
8 https://publichealth.gwu.edu/content/women-remain-underrepresented-medical-science-new-report-says
9 https://www.heart.org/en/news/2019/04/04/proactive-steps-can-reduce-chances-of-second-heart-attack
10 https://www.cdcfoundation.org/blog/cdc-foundation-million-hearts-and-partners-spotlight-cardiovascular-disease-during-covid-19
11 https://www.cdc.gov/mmwr/volumes/69/wr/mm6925e2.htm
12 https://www.bayer.com/en/personal-health/protecting-heart-health











