How Close Are We to Finding a Treatment for COVID-19?

Scientists are following several paths in the battle with COVID-19 as they seek to help treat patients in the short term and protect the population in the future.
The global pandemic has prompted possibly the largest and fastest mobilization of the global scientific community we’ve ever seen. Researchers are working around the clock to find a solution, trials are being initiated at record speed, and businesses are offering up their resources to help in any way they can. It has been a collective response encompassing governments, academia, charities, the pharmaceutical industry, and local communities. But with all that effort, how close are we to a developing a drug to treat or prevent COVID-19?
When it comes to new treatment options, there are three routes that can make a difference for patients both in the near- and mid-term: developing a new vaccine; replicating the antibodies that fight the virus; repurposing existing drugs that might be effective.
The reason for following all of these paths is that they take differing amounts of time to achieve. Developing a drug from scratch can take years while discovering that an existing approved drug is effective can be a matter of weeks. And this is critical for helping seriously ill patients as soon as possible.
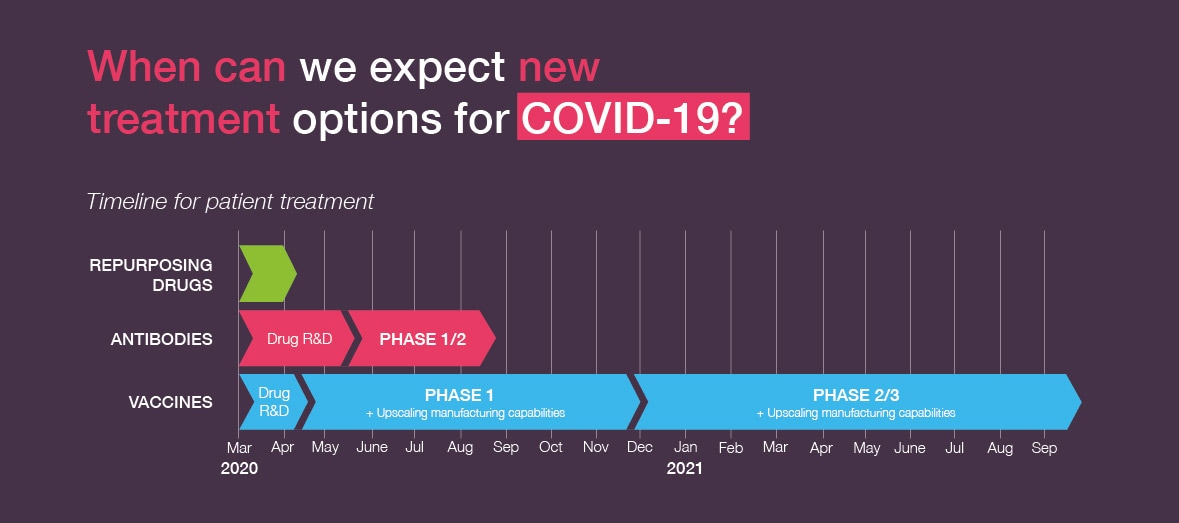
Repurposing Existing Drugs
Timeline: Available now, but efficacy and safety testing could take until summer
Scientists are looking at repurposing existing drugs that might either fight the virus directly or help reduce the overreaction of the immune system that can occur when the body is fighting the virus and can lead to the hospitalization of patients. The advantage of researching existing approved drugs is that we know they have a well described benefit-risk profile in the indications they are approved for and have already been produced at scale. This means that – if they are found to be effective for other indications – they could quickly be repurposed to help a large number of people.
To identify which drugs would work, scientists mapped the interaction between the virus and human proteins to understand which cells were targeted. This provided a starting point for understanding how the virus fights off the immune system and which existing drugs might be effective.
A number of drugs are being looked at from anti-virals to antimalarials to immunomodulatory agents, which could help to reduce severe immune overreactions. In March, the World Health Organization launched an international clinical trial called Solidarity to speed up the process of finding an effective treatment for COVID-19. The Solidarity trial is comparing four treatment options: Chloroquine – which Bayer markets in Pakistan under the brand name Resochin® – and Hydroxychloroquine (used to treat malaria and rheumatology conditions respectively); Remdesivir (developed as a treatment for Ebola); Lopinavir/Ritonavir (a licensed treatment for HIV); Interferon beta-1a (sed to treat multiple sclerosis).
The key now is for rigorous clinical trials to take place over the next few weeks to see whether these drugs are safe and effective for patients, with the results due over the next couple of months. For example, Bayer partnered with the Population Health Research Institute (PHRI) in launching a major clinical research program aimed at identifying potential treatments against COVID-19. The two studies will evaluate the safety and efficacy of different combination therapies including Bayer's chloroquine and interferon beta-1b.
Using Antibodies Against the Virus
Timeline: Potentially early fall
When a virus attacks us, our immune system produces Y-shaped antibody proteins to latch on to the virus and neutralize it. For COVID-19, that means people who have successfully recovered from the disease have produced antibodies to stop the coronavirus in its tracks. Scientists have been working on identifying and reproducing those antibodies as a treatment.
Small scale tests in China found that critically ill patients could benefit from infusions of blood plasma collected from people who have recovered. However, people differ in their immune responses and will produce different levels of antibodies. This is why there are several types of antibody treatments being developed beyond using recovered patient blood plasma.
One concept is to genetically engineer laboratory mice to mimic the human immune system, expose them to the coronavirus and collect the virus-blocking antibodies from the recovered animals. By doing this in a controlled environment, scientists can better understand and engineer the process.
Another method is to create synthetic antibodies. This is done through isolating the antibody producing white blood cells from the blood of recovered patients, copying their DNA and reproducing it. The antibodies which are most effective against the virus can then be identified and mass manufactured. Other biotech companies are using computers and artificial intelligence to reengineer and optimize antibodies that are known to target the coronavirus behind the 2003 outbreak of SARS,
SARS-CoV-1.
A different approach is not to use antibodies directly, but to stimulate their production in the patient's cells. To do so they would develop an active ingredient from messenger RNA (a molecule which carries the genetic code for a particular protein) to promote the body's production of antibodies.
Several of these projects are now in clinical trials with the hope they could be available by fall.

Finding a Vaccine
Timeline: Potentially first half 2021
The ultimate aim is to create a vaccine so that we can not only treat but prevent COVID-19 returning in the future. However, developing an effective vaccine has traditionally taken years. Compressing this to months has taken global collaboration and significant investment.
According to the Milken Institute tracker, there are more than 240 vaccines currently in development, with many candidate vaccines currently heading toward or already in clinical trials. If proven effective, any of those vaccines would likely become widely available by 2021.
While great strides in developing experimental vaccines have been made, there are still plenty of hurdles. To confirm that a medicine is safe and effective, we need to run large, controlled studies across different populations of patients. This means any new vaccine will have to go through three clinical phases before being licensed.
Once we have a working vaccine in hand, companies will need to start producing millions — perhaps billions — of doses, in addition to the millions of vaccine doses that are already made each year for mumps, measles and other illnesses. We will need to find new ways to rapidly scale manufacturing around the world.
An unprecedented public health crisis has led to an unprecedented global response where Bayer makes a significant contribution (see box below). While the world searches for a vaccine, in the short term our best hope for patients may be in identifying existing medicines that can effectively combat COVID-19.
Bayer’s Contribution to Combat
COVID-19
As a company active in the areas of health and nutrition, we can provide substantial help in overcoming the crisis with our products and our expertise. Here is what we do to find potential treatment options.
We are pursuing a number of approaches to support people suffering from COVID-19 and help ease the pressure on overwhelmed health systems.
One example is chloroquine (trade name: Resochin®), a long-used malaria drug from Bayer. The Chinese health authorities have included it in the treatment recommendations for COVID-19. Subsequently, many other health authorities have adopted similar guidance.
Resochin has been shown to reduce the viral load in the laboratory and in initial clinical trials and might help in treating patients. However, its effectiveness against COVID-19 requires further testing. Larger-scale clinical studies are now being launched, including by the WHO, to carry out a risk-benefit assessment for the use of chloroquine to treat people with COVID-19. The scientists hope to gain meaningful results in the coming weeks.
Because patient safety is of utmost importance, Bayer is exclusively providing study drug to clinical trials and donating product to governments to allow for a coordinated and supervised emergency use of chloroquine outside of established indications.
In addition to looking into the potential of Resochin, we’re assisting in the search for a new active substance to treat COVID-19. This includes unprecedented collaboration with all our stakeholders including other pharmaceutical companies.
We are in scientific discussions with institutions to explore potential benefits of other Bayer compounds against COVID-19.And, we’re providing access to our substance library and conducting screening work to find a potential active ingredient. Bayer is part of the COVID-19 Therapeutic Accelerator Initiative run by the Bill & Melinda Gates Foundation and is actively supporting the research program by the Population Health Research Institute (PHRI) at McMaster University, Canada, by providing study drug and financial support. In addition, we are contributing to the search for an active substance to treat COVID-19 as part of the Innovative Medicines Initiative (IMI).
We are also committed to contribute to the production of a possible vaccine against the coronavirus, if it is successfully tested and approved.
Bayer currently doesn’t manufacture vaccines, but we are intensively working on options how we could use our company’s resources and capacities to support the increasing demand in the space of mRNA vaccines.
These examples serve to highlight how we are using our knowledge and capacities to combat COVID-19. Further, we want to ensure that this health crisis does not turn into a hunger crisis. We will continue to do whatever we can to fight the spread of the virus and work toward our vision: “Health for all, hunger for none”.
Find out more about all our activities to fight the coronavirus at bayer.com/corona








